As I lifted my son Felix up over my shoulder for his standard burping stint after our midnight feed last Friday evening, he started to cough. I paused: normally he would burp, maybe spit, and the limit have some milk dripping out of his nostril. But he didn’t cough. I listened to him after placing him back in his bassinet, worrying there was something off. His breathing rattled raucous. I barely slept. A few hours later, at our 3:00 am feed, he coughed again. I alerted my husband that I worried something was wrong. We waited until morning. Normally, Felix is massively alert from about 9:00 am to 10:30 am. He plays Japanese war history with his father as I make breakfast for the two of us. But on Saturday he was lethargic. We tried to rouse him, but he stayed asleep. I called our midwife, called the family doctor’s office, called the resident on call at the hospital. By the time they responded, we had made a decision to bring him to the emergency room. He didn’t open his eyes while I put on his blue bear suit on the changing table, to keep him warm in the cold April wind outside. It was all I could do to stop my own tears, to maintain composure as the fear set in.
I projected a future state where all I had of him were the few pictures I’d put up on Facebook. Where all we were given was 5.5 weeks. Where all that would remain would be the memories of how active his breathing became when he concentrated, of the way he laid his head on his hands to sleep on my chest after a feed. I cried over this feared future and realized just how deeply I love him.
The parking lot at the hospital was surprisingly empty. Back during our prenatal visits in January and February we had to fight for parking spots, adding an additional 15 minutes travel time to make sure we were on time. We skipped the parking fee to save time and walked as quickly as possible to the hospital entrance. In front of the normal revolving door stood two temporary entrances: one for patients and visitors and one for staff. We walked through the first. The light changed from sun to dark. A few masked hospital attendants were seated at a greeting table. Upon seeing a small infant wrapped in my arms, hearing my cry that our son wouldn’t rouse, they rushed us to a screening from in the ER. We sanitized our hands and put on face masks. Walked through the bottom foyer spotted with a few people, some ordering coffee from Second Cup, some sitting like sentinels in masks monitoring the surroundings. We moved fast. Walked to a nursing station where four of five nurses looked at my son. “He’s still pink,” they said. “That’s a good sign. But we can’t care for him here. You should take him across the street to SickKids.”
We turned. Back through the corridor and across the street. I did everything I could to keep his head warm from the wind. Mihnea, my partner, reminded me it was more important to keep his airways open at this time. Our pupils resettled again as we entered the SickKids entrance. My glasses fogged from the humidity rising from my mouth through the mask. “I can’t see anything,” I said to Mihnea. He took off my glasses and wiped them as I walked to the line to register our son for care. The attendant asked me three screening questions and checked boxes on a form: Have you traveled to a foreign country in the last 14 days? Do you have any of the following respiratory symptoms? “Only one support person is allowed in with the child.” I told Mihnea it was me. He said he would try to get water-only baby wipes while we were in the hospital. I barely said goodbye, rushing to get my son care.
They put a hospital band around his tiny wrist and again comforted me that things couldn’t be dire because his color was still ok. I described his symptoms, answered another screening questionnaire about my own respiratory symptoms. And we were escorted down the hall into room number 7, waiting for the nurse and doctor to arrive.
The nurse came first. He was calm as they took his vitals, lethargic from the illness. Heart and breathing were normal. No audible congestion in the lungs. No fever. We stripped him naked and weighed him: 4.69 kilos, or 10 pounds 5.4 ounces. He’d grown a ton since his weight dropped to 6 pounds 8 ounces during the early-day dip in the hospital, fed only on colostrum from breasts getting practice with breastfeeding. The nurse asked if I’d like to turn the overhead light down. “Sure,” I said, settling into the dim darkness, obsessively scanning the white bars of the hospital crib as I held my son in my arms waiting for the doctor to arrive. I asked if they had diapers and wipes, as he needed to be changed. No wipes, but they did offer 2 size 1 diapers. They were scented: I cringed, as I only allow my son to wear diapers that are pure. But there was no choice. We wiped him with a paper towel and little water, leaving some residue on his bum. Again, this wasn’t the time for me to fuss.
The doctor came shortly thereafter. An Indian woman who exuded wisdom, practice, and care. She asked questions, listened to the rasp in Felix’s breathing as I rocked him, waited a little until she could hear a cough. Was encouraged that his vital signs were ok, and requested that I stay in the hospital through a couple of feeds to monitor how things progress. “It’s tricky with little ones,” she said. “If you’re worried, we’re worried. Symptoms progress rapidly in one or the other direction, so let’s watch him and see what happens.”
“Ok,” I responded, laconic. “Do you have any food or water for me while I wait?” I am meticulous about my hydration and nutrition while breastfeeding my son. Drink liters of water per day. Eat incredibly well.
“I can bring you a cup of water and a nutrigrain bar. If you need a proper meal, we can see to that later.”
She returned with a small styrofoam cup filled with tap water, 2 nutrigrain bars (one blueberry and one mixed berries), and 2 packets of shortbread cookies. I asked if she could watch Felix while I went to the bathroom. She offered to hold him, cradling him against the yellow gown over her chest.
She passed him to me and closed the curtain behind her as she left. I downed the 6 ounces of water from the styrofoam cup and plugged in my cell phone. And I sat in a hunter green plastic chair, holding my son. They’d removed the comfy nursing chairs because they are harder to sterilize during COVID.
Hours passed. I looked at the white bars on the hospital crib. Paced around the room to relieve my aching back. Held my son. Was bothered by the sickly smell of the scented diaper. Spoke to Mihnea and my parents on the phone. Responded to a few texts I’d been meaning to respond to, mentioning to an old friend that we were in the ER. Nothing to read. Nothing to eat. I was in my pyjamas, as I didn’t make time to change before we left: grey Quantas airline sweatpants my mother got on a trip back in the 1990s, the drawstring still in the pants under tatters of revealed seams; Mihnea’s grey Burberry shirt with four buttons near the collar, undone so I could feed; no bra; hiking boots; a grey sweatshirt stained with spit up and leaking breast milk I took off and laid on the green plastic chair next to me so Felix wouldn’t get wet. We didn’t have any extra outfits for him. Nothing. I needed to keep him dry.
Eventually, he ate. It was a tired feed, lacking his normal vigor. He sneezed and coughed, but didn’t pull off. I took videos of his sounds to show the doctor.
She returned to check in a few times and eventually we did another examination. And, fortunately, he stirred. “Look at his eyes!,” she exclaimed. “He is beautiful. Strange that the first images he’ll form will be of people will be with masks.”
She was encouraged by his energy, but offered a COVID swab. I accepted. The nurse came in with what looked like a small white sword, the size of a cocktail umbrella. While Felix had roused a little, he was still drowsy so more tolerant of sticking a swab up his nose than he normally would be. I embraced him. She stuck it up the right nostril. He cried a little, but not too badly. She stuck it up the left. And that was it. “Can I hurt him?” I asked. “No,” she replied. “You’ll have results in 2-4 days.”
Because Felix was showing signs of improvement, the doctor felt comfortable discharging us around 5:00 pm, about 5 hours after we arrived. She diagnosed him with a viral respiratory infection and gave instructions on waiting for the COVID test result. Made a virtual check-in with a pediatrician the following day. “Are there any concerns I can help address?” she asked.
“My biggest worry is that I will lose my son,” I replied.
“We’ll act on him before that happens. Put him on an IV or oxygen support. What matters is that if you’re worried, we are worried. Symptoms with little ones progress quickly, and you know better than anyone if he is behaving differently from normal. Look out for signs of breathing distress, fever, dehydration, vomiting. But some congestion is ok. Good luck!”
I dressed Felix back in his big, warm, blue bear suit. Mihnea came and picked us up, holding Felix closely to his chest as we greeted us at the entrance where he’d left us that morning.
We drove home, vigilant. We ate dinner, vigilant. We slept next to him in our bed, vigilant. We fed him, vigilant.
He got better. Quickly.
We got a call within 20 hours informing us that his COVID test results were negative, but that, given the potential for a false negative, he should still be isolated for 3-4 days. We wouldn’t have brought him for a walk in the cold anyway. Homebound, vigilant.
The experience upended us. We learned to cherish his wails, as they signaled vigor and life. To cherish the frustrations of being tired as he still doesn’t sleep more than 3 hours at a time at night (but it’s getting better and better!). To cherish his clear breathing. To cherish the raw fact of his existence. To cherish that he is our son. We always did, but we do now more than ever.
There is no science to newborn care. It’s a matter of intuition. States change in a matter of hours, and a parent is tasked with watching severity, not duration. I wanted guidelines, measurements, answers. There were none. Just the amazing burden of responsibility to know another deeply, to know Felix inside out and backwards and know when it could be time to bring him back to the hospital for additional care.
It’s as I mentioned in my last post: a recipe for misery is to compare your child with statistical development milestones. Parenting is about depth of knowledge, the depth of knowing one little person in every aspect of their being. I have deepened my knowledge of the rate and cadence of his breathing. Of his body temperature. Of his moods. Of the hint of redness that appears around his eyes when he is sick. Of the wetness of his tears and the inside of his mouth. Of the way his hands move when he is curious and when he is scared. Of the feelings that emerge in the bath, on the bed, on his play mat. He is my world now. Our world. The only way to care for a sick newborn is to pay close attention to who he is and how he is. And to know when he’s not himself.
I will hold deep inside me a token of unconditional love in the backache I felt sitting in the dark against a plastic green chair in a hospital room on a Saturday afternoon. There was no question I would do otherwise, as I will when, inevitably, the next worry comes our way.
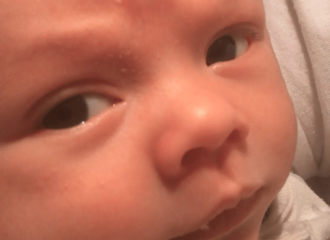
The featured image is of my son Felix this Saturday morning. I can see the illness in the little tear grazing the bottom of his eye, the depth and sadness in his plea. He couldn’t voice his pain, couldn’t tell us what was coming. All we could do was listen.